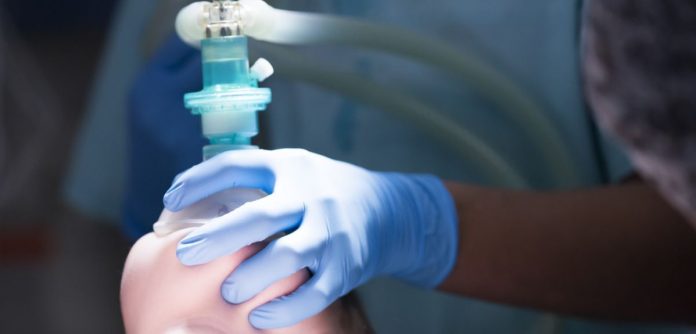
General anaesthesia is widely used for surgery and diagnostic interventions, to ensure the patient is completely unconscious. But it is not used generally for dying patients, to whom painkilling medications (analgesia) are more commonly given. But, according to the paper, this may not be enough, leading to the use of continuous deep sedation, also known as palliative or terminal sedation.
Professor Julian Savulescu, Oxford’s Uehiro Chair of Practical Ethics and co-author, maintains, ‘For some patients these common interventions are not enough. Other patients may express a clear desire to be completely unconscious as they die.’
He adds, ‘Some dying patients just want to sleep. Patients have a right to be unconscious if they are dying. We have the medical means to provide this and we should.’
The authors make clear their proposal is not about assisted dying, currently illegal in the UK. Instead, their focus is on options to ensure patients are comfortable at the end of their lives.
Dr Jaideep Pandit, Professor of Anaesthesia at Oxford University Hospitals NHS Foundation Trust, and a co-author, says, ‘The desire to be unconscious as a means of eliminating the experience of physical or mental suffering is understandable.
‘Unconsciousness through general anaesthesia offers the highest chance of making sure that the patient is unaware of going through an adverse process.’
He adds, ‘Although general anaesthesia in end-of-life care has been used and described in the UK since 1995, modern multidisciplinary guidelines will be needed before this can be offered more widely. Raising this issue now is important, especially in view of international trends showing increased use of general anaesthesia for dying patients.’
Informed consent will, say the authors, be crucial in helping patients understand implications of general anaesthesia for end-of-life care, and their other options to manage their final days.
Professor Dominic Wilkinson, Director of Medical Ethics at the Uehiro Centre, and a co-author, says, ‘It is vital that patients are informed of all the legal options available to them to relieve suffering at the end of life. That includes analgesia, sedation and, potentially now, anaesthesia.
‘The risks and benefits of each should be explained. Patients should be free to choose the option, or combination of options, that best meet their values.’
In a separate survey, published recently, Professors Wilkinson and Savulescu found a high level of support for access to deep sedation in dying patients. Some 88% of those surveyed said they would like the option of a general anaesthetic if they were dying. About two thirds (64%) said they would personally choose to have an anaesthetic at the end of life.
Professor Wilkinson maintains, ‘Members of the general public appear to value the option of deep sleep and complete relief from pain if they were dying. Our previous research indicates that the public believes that patients should be given this choice.’
The authors reject concerns that the use of general anaesthesia for end-of-life care could hasten death. Studies show no statistically significant difference in mean survival time between patients at the end of life who receive continuous deep sedation and those who do not. In several countries, propofol infusion, as used for general anaesthesia, has been continued for up to 14 days.
‘This stresses the point that the purpose of administering anaesthesia is not to hasten death but simply to achieve unconsciousness,’ explains co-author Antony Takla, Research Associate at the Uehiro Centre.
The authors believe the UK medical community should prepare for increased requests for general anaesthesia for end-of-life care, based on current trends in Western Europe and Scandinavia.
The paper concludes, ‘We have described a potential role for general anaesthesia in end-of-life care. This has, in reality, been available to UK patients since the 1990s, but is not commonly discussed or provided. There is a strong ethical case for making this option more widely available. This does not imply that existing palliative care practice is deficient. Indeed, we might see that general anaesthesia in end-of-life care is requested by, or suitable for, very few patients.
‘However, the number of patients involved should not alone determine whether this issue is regarded as ethically important. Even if complete unconsciousness is desired by only a few patients, there is a moral imperative for national anaesthesia, palliative care and nursing organisations to prepare for the possibility that general anaesthesia in end-of-life care may be requested by some patients, and to work collaboratively to develop clear protocols to address all of the practical, ethical and medicolegal issues concerned.’