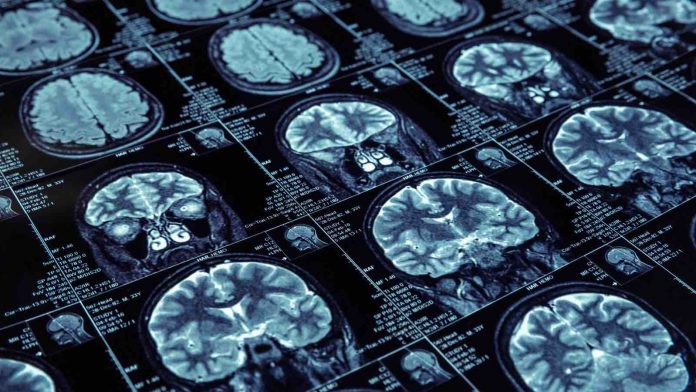
What’s the connection between inflammation, how much your brain may shrink each year, and insulin resistance? Last year in the Sacramento and Davis regional area, a study at U.C. Davis revealed that the human brain tends to shrink with age. This can’t be entirely prevented by nutrition changes. However, there are a few things that clearly affect brain atrophy.
Read more about the UC Davis research, Study Reveals Why Brain Shrinks With Age. And check out, Controversial Brain Shrinkage Study CBS. This controversial study from U.C. Davis looked at brain shrinkage and health conditions such as diabetes, obesity, and hypertension.
The study at the University of California at Davis made new headway in determining the factors that affected brain degeneration. The study concluded that individuals who made certain life decisions or suffered from medical conditions such as hypertension, diabetes, obesity, and a smoking habit were more likely to suffer from degeneration.
Diabetic brain shrinkage can be lowered
At the age of 65, the average person’s brain shrinks about one percent a year. But in a diabetic patient, brain volume can be lowered by as much as 15 percent.
The study concluded that individuals most at risk of suffering from atrophy were those who smoked, suffered from diabetes, had high blood pressure or were overweight. In the UC Davis study, people with any of these health complications in midlife were more likely to develop dementia later on in life.
Hypertension and dementia
The study revealed that individuals with high blood pressure in their fifties could experience dementia in less than a decade. If drugs aren’t helping your blood pressure, maybe you should look into other ways to lower your blood pressure. One of those ways could be alternative medicine or food as medicine.
Another could be an implant, if drugs fail to work. And some people walked away from conventional medicine altogether and tried a medley of alternatives finding something that works for them, including slow music, nutrition changes, and various activities or lifestyle changes, even art or slow music and slow breathing therapy to relax.
Insulin resistance and alternative nutrition
On the other hand, one of the advantages of alternative medicine in looking at ways to help your insulin resistance before you have to depend upon prescription drugs to survive is that it affords the individual the broadest range of health treatment options, provided that you know the consequences of what you’re thinking of doing.
One question scientists ask in numerous studies is whether the result of diabetes and/or insulin may be cognitive dysfunction in later years? A new study now has found that insulin resistance may be associated with inflammatory processes that lead to cortical atrophy and brain dysfunction. Now there’s another study linking diabetes to cognitive impairment in older individuals.
Diabetes link to cognitive impairment in older adults
“Researchers identify diabetes link to cognitive impairment in older adults.” Many complications of diabetes, including kidney disease, foot problems and vision problems are generally well recognized. But the disease’s impact on the brain is often overlooked. See the journal Diabetes Care.
For the past five years, a team led by Beth Israel Deaconess Medical Center (BIDMC) neurophysiologist Vera Novak, MD, PhD, has been studying the effects of diabetes on cognitive health in older individuals and has determined that memory loss, depression and other types of cognitive impairment are a serious consequence of this widespread disease.
Now, Novak’s team has identified a key mechanism behind this course of events, according to the news release. In a study published in the November 2011 issue of the journal Diabetes Care, they report that in older patients with diabetes, two adhesion molecules – sVCAM and sICAM – cause inflammation in the brain, triggering a series of events that affect blood vessels and, eventually, cause brain tissue to atrophy. What about the rapid rate of brain shrinkage in diabetics after age 65?
Importantly, they found that the gray matter in the brain’s frontal and temporal regions — responsible for such critical functions as decision-making, language, verbal memory and complex tasks – is the area most affected by these events.
Who gets more brain atrophy?
“In our previous work, we had found that patients with diabetes had significantly more brain atrophy than did a control group,” explains Novak, Director of the Syncope and Falls in the Elderly (SAFE) Program in the Division of Gerontology at BIDMC and Associate Professor of Medicine at Harvard Medical School, according to the news release. “In fact, at the age of 65, the average person’s brain shrinks about one percent a year, but in a diabetic patient, brain volume can be lowered by as much as 15 percent.”
Diabetes develops when glucose builds up in the blood instead of entering the body’s cells to be used as energy. Known as hyperglycemia, this condition often goes hand-in-hand with inflammation.
Novak wanted to determine if chronic inflammation of the blood vessels was causing altered blood flow to the brain in patients with diabetes
To test this hypothesis, Novak’s team recruited 147 study subjects, averaging 65 years of age. Seventy one of the subjects had type 2 diabetes and had been taking medication to manage their conditions for at least five years. The other 76 were age and sex-matched non-diabetic controls.
Study subjects underwent a series of cognitive tests, balance tests and standard blood-pressure and blood-glucose tests. Serum samples were also collected to measure adhesion molecules and several other markers of systemic inflammation.
To determine perfusion (blood flow) measures in the brain, patients also underwent functional MRI testing, in which a specialized imaging technique known as arterial spin labeling (developed by BIDMC MR physicist David Alsop, PhD) was used in conjunction with a standard MRI to measure vascular reactivity in several brain regions and to show changes in blood flow.
Diabetics and blood vessel constriction
As predicted, the scans showed that the diabetic patients not only had greater blood vessel constriction than the control subjects, but they also had more atrophied brain tissue, particularly gray matter. The results also showed that, in the patients with diabetes, the frontal, temporal and parietal regions of the brain were most affected. Similarly, the team’s measurements of serum markers confirmed that high glucose levels were strongly correlated with higher levels of inflammatory cytokines.
“It appears that chronic hyperglycemia and insulin resistance – the hallmarks of diabetes – trigger the release of adhesion molecules [sVCAM and sICAM] and set off a cascade of events leading to the development of chronic inflammation,” says Novak. “Once chronic inflammation sets in, blood vessels constrict, blood flow is reduced, and brain tissue is damaged. ”
Biomarkers
This discovery now provides two biomarkers of altered vascular reactivity in the brain. “If these markers can be identified before the brain is damaged, we can take steps to try and intervene,” says Novak, explaining that some data indicates that medications may improve vascoreactivity.
But more important, she says, the new findings provide still more reason for doctors and patients to focus greater attention on the management – and prevention – of diabetes. “Cognitive decline affects a person’s ability to successfully complete even the simplest of everyday tasks, such as walking, talking or writing,” says Novak.
Type 2 diabetes: Effects on the brain
“There are currently 25.8 million cases of type 2 diabetes in the United States alone, which is more than eight percent of our total population. The effects of diabetes on the brain have been grossly neglected, and, as our findings confirm, are issues that need to be addressed.”
This study was supported, in part, by grants from the National Institute of Aging, the National Institute of Diabetes, Digestive and Kidney Diseases, the American Diabetes Association, and the National Center for Research Resources.
Study coauthors include BIDMC investigators Peng Zhao, PhD, Brad Manor, PhD, Ervin Sejdic, PhD, David Alsop, PhD, and Medha Munshi, MD; Amir Abduljalil, PhD, of Ohio State University; Paula Roberson, PhD, of the University of Arkansas for Medical Sciences; and Peter Novak, MD, PhD, of the University of Massachusetts Medical School.
Beth Israel Deaconess Medical Center is a patient care, teaching and research affiliate of Harvard Medical School and ranks third in National Institutes of Health funding among independent hospitals nationwide. BIDMC is a clinical partner of the Joslin Diabetes Center and a research partner of the Dana-Farber/Harvard Cancer Center. BIDMC is the official hospital of the Boston Red Sox.