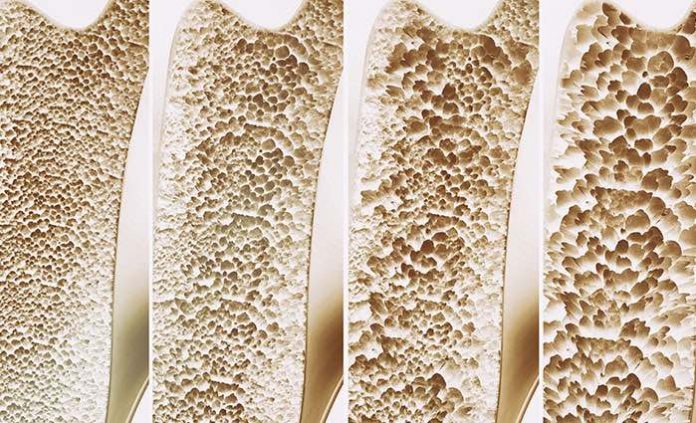
To reduce the risk of bone fractures and the associated complications, the United States Preventive Services Task Force (USPSTF) recommends that all women age 65 and older be tested and treated for low bone mineral density. In addition, the USPSTF recommends that postmenopausal women aged 50 to 64 should have bone mineral density screenings if their 10-year probability of suffering a hip, vertebral, humerus (upper arm) or wrist fracture is 9.3% or higher, based on the Osteoporosis Self-Assessment Tool (OST).
A new UCLA-led study has found that the USPSTF recommendations have a major flaw. It reported that the guidelines predicted only slightly more than 25% of the women who went on to experience major osteoporotic fractures within 10 years. In addition, the study found that two older osteoporosis risk-assessment tools were not much better. The findings were published online on October 16 in the Journal of Clinical Endocrinology & Metabolism.
The OST is based on a person’s weight and age, and the Simple Calculated Osteoporosis Risk Estimation Tool (SCORE), uses race, rheumatoid arthritis, history of non-traumatic fracture, age, prior estrogen therapy, and weight. “If we want to prevent fractures, we need tools that help us accurately predict who will suffer these osteoporotic injuries so that we can target these at-risk people for preventive measures,” explained primary investigator Dr. Carolyn Crandall, professor of medicine in the division of general internal medicine and health services research at the David Geffen School of Medicine at UCLA. She added, “Our results suggest that our current guidelines for screening in younger post-menopausal women do not accurately identify who will suffer a fracture.”
For the study, the investigators accessed data from the Women’s Health Initiative, which collected specifics about fractures during a decade and information about osteoporosis risk factors from 62,492 postmenopausal women in the US from ages 50 to 64. Of the study group, 85% were white, 9% were black, and 4% were Hispanic. The average age was 57.9 years. The researchers found that overall the USPSTF strategy identified only 25.8% of the women who suffered fractures within 10 years, SCORE identified 38.6% and OST caught 39.8%.
These were the findings for the percentage of women whose fractures were predicted using each risk-assessment tool for three age groups:
Ages 50-54 Ages 55-59 Ages 60-64
USPSTF 4.7% 20.5% 37.3%
SCORE 18.5% 22.1% 57.6%
OST 22.9% 36.7% 48.1%
The authors pointed out a weakness of the study: the participants of the Women’s Health Initiative may be healthier than similarly-aged women physicians see in their clinical practice; therefore, the findings may not generalize to others. Despite that weakness, the findings suggest that the current USPSTF screening strategy does not identify the vast majority of younger post-menopausal women who experienced bone fractures; furthermore, the other strategies have significant weaknesses as well.
The authors wrote: “Neither the USPSTF nor the other two screening strategies performed better than chance alone in discriminating women who did and did not have subsequent fractures. “These findings highlight the pressing need for further prospective evaluation of alternative strategies with the goal of better targeting resources to at-risk young postmenopausal women. Our findings do not support use of the USPSTF strategy or the other tools we tested to identify younger postmenopausal women who are at higher risk of fracture.”